Ramblings from Red Shift this week takes a look at Ehlers-Danlos Syndrome (EDS), a group of rare inherited conditions that affect connective tissue. Why take a look at such a rare condition? Well, Susie was telling me how two patients with EDS had just attended the same emergency department at the same time – the odds of which are pretty unlikely – and that reminded me of a patient with EDS we used to regularly see in the UK. The patient’s address had a warning information alert for all ambulance crews – although you generally didn’t forget if you had attended previously. In majority of cases, she required a hospital pre-alert and a priority 1 journey to hospital – I think her intubation record stood at 36 times in 24 years. Specific risks for patients with EDS in emergency situations include:
- spontaneous arterial rupture or dissection (primary cause of mortality);
- pneumothorax, pneumo-mediastinum: spontaneous or iatrogenic (for example caused by mechanical ventilation);
- bowel rupture;
- pulsating exophthalmos (bulging of the eye out of the socket) due to formation of a carotid-cavernous fistula;
- uterine rupture during pregnancy, delivery or the post-partum period.

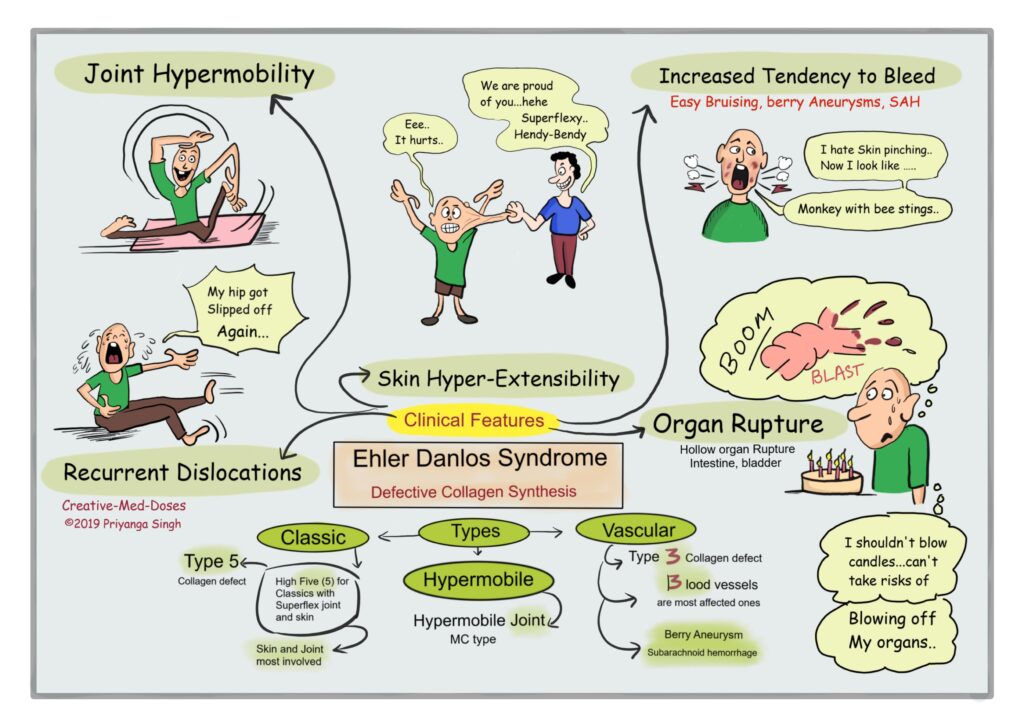
The Ehlers-Danlos syndromes are a group of connective tissue disorders that can be inherited and are varied both in how they affect the body and in their genetic causes. They are generally characterised by joint hypermobility (joints that stretch further than normal), skin hyperextensibility (skin that can be stretched further than normal), and tissue fragility.
There are 13 types of EDS, most of which are very rare. Hypermobile EDS (hEDS) is the most common type and Vascular EDS is considered the most serious.
Hypermobile EDS. People with hEDS may have:
- joint hypermobility;
- loose, unstable joints that dislocate easily;
- joint pain and clicking joints;
- extreme tiredness (fatigue);
- skin that bruises easily;
- digestive problems, such as heartburn and constipation;
- dizziness and an increased heart rate after standing up;
- problems with internal organs, such as mitral valve prolapse or organ prolapse;
- problems with bladder control (stress incontinence).
Vascular EDS. Vascular EDS (vEDS) is a rare type of EDS and is often considered to be the most serious. It affects the blood vessels and internal organs, which can cause them to split open and lead to life-threatening bleeding. If a patient with vEDS presents with signs of chest or abdominal pain it should be considered as potentially serious trauma. People with vEDS may have:
- skin that bruises very easily;
- thin skin with visible small blood vessels, particularly on the upper chest and legs;
- fragile blood vessels that can bulge or tear, resulting in serious internal bleeding;
- a risk of organ problems, such as the bowel tearing, the womb tearing (in late pregnancy) and partial collapse of the lung;
- hypermobile fingers and toes, unusual facial features (such as a thin nose and lips, large eyes and small earlobes), varicose veins and delayed wound healing.
And why the Zebra on the EDS artwork? During medical school, students are often told “when you hear hoof beats, think horses, not zebras’. In medicine, the term ‘zebra’ is used in reference to a rare disease or condition. Doctors are taught to assume the simplest explanation is usually the best, so as not to go around diagnosing patients with all sorts of rare exotic diseases that are highly unlikely – common diseases are more likely the diseases most likely encountered. EDS is considered a rare disease, so EDS sufferers are medical zebras – the zebra is actually the logo of The Ehlers-Danlos Society.
Information on managing Vascular EDS emergencies can be found here:
EDS emergency advice for healthcare staff:
General information on EDS from The Ehlers-Danlos Society.

