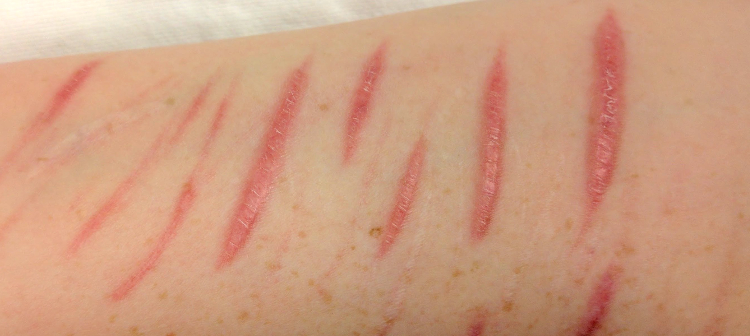
It’s three AM and you receive a call to a 23 year old female who is not coping and has cut herself. Your colleague loudly vocalises that she has probably only scratched herself, wants some attention and that it’s a crap, waste-of-time call. Admittedly, when starting in this career, I remember joking that perhaps the ambulance service should run seminars entitled ‘Suicide: how to do it properly’, but that was before taking the time to talk to patients on their reasons for self-harm in an attempt to understand their mindset, and also personally experiencing the darkness that can be associated with the human mind. According to National Institute of Health and Care Excellence (NICE) guidelines, ambulance staff should be trained in the assessment and early management of self-harm. Training should particularly address: the different methods of self-harm and the appropriate treatments: the likely effects if untreated: and issues of consent and mental capacity, as these apply both to adults and to children and young people.
While in many cases self-harm is not intended to be fatal, it does need to be taken seriously. For some, the function of self-harm is a way to alleviate intense emotional pain or distress, or overwhelming negative feelings, thoughts, or memories. For others, it’s a form of self-punishment, to end experiences of dissociation or numbness, or as a way to show others how bad they feel. While it may seem counter-intuitive, self-harm is used as a coping mechanism rather than a suicide attempt.
Self-harm proved to me I was real, I was alive. At times it also silenced the chaos in my head, briefly pausing the repetitive flashbacks and body memories.
Self-harm is actually a serious public health issue. Taken together, suicide and self-harm account for a considerable portion of the burden of disability and mortality among young people. Worldwide, in those aged 10-24 years, self-harm is the seventh leading contributor to the burden of disease in both males and females. According to an Australian report into youth mental health, 24.4 per cent of young women and 18.1 per cent of young men aged 20-24 have self-injured in their lifetime. Examining young Australians’ health and well-being, non-fatal suicidal behaviour and self-harm are associated with substantial disability and loss of years of healthy life.
There is still terrible misunderstanding and stigma associated with self-harm, resulting in damaging responses from the wider community – including health professionals. Unsympathetic, unhelpful or dismissive responses from healthcare professionals can create a far greater harm than any physical injury they have inflicted upon themselves. Making them feel worse about their situation deters them from asking for help in the future, increasing the likelihood of future adverse outcomes. Just one bad experience can lead to the patient never asking for help again.
Self-harming behaviours are often in response to intense emotional or physical pain and psychological distress, including overwhelming negative feelings, thoughts or memories, and a sense of hopelessness. For some, self-harming can have an addictive element, possibly due to the natural release of endorphins in response to pain, and possibly due to a lack of alternative coping strategies. People who self-harm have genuine difficulties coping with aspects of their lives. Only in some cases is self-harm is accompanied by suicidal ideation.
Self-harm is definitely not just attention seeking, many people who self-harm hide their wounds and scars. It is estimated that over 50 per cent of young people do not actually seek help, and actively attempt to conceal their behaviour. Some hide through the use of clothing, such as gloves, long sleeved clothes and scarfs, while others become withdrawn and avoid personal contact. Embarrassment and refusal (either by the patient or others) to acknowledge self-harm as a form of mental ill-health can be just some of the reasons why they don’t ask for help.
While cutting is one of the most common forms of self-harm, the range of different types is huge – just think of the various ways possible to hurt yourself, both physically or mentally. Ways of self-harm can also include poisoning or over-dosing; over and under-eating; hitting or biting themselves; picking, scratching or burning their skin; exercising excessively; and getting into fights where they know they will get hurt.
The reasons for self-harm can be as varied as the types of self-harm, some people have described self-harm as:
- a way to express something that is hard to put into words;
- a way to turn invisible thoughts or feelings into something visible;
- changing emotional pain into physical pain, for example, releasing the pent-up emotional pain, frustrations or anger by burning or cutting to create physical injuries that can be seen and felt its like releasing the pressure;
- reducing overwhelming emotional feelings or thoughts;
- having a sense of being in control;
- an escape from traumatic memories;
- having something in life that they can rely on;
- a form of punishment for feelings and experiences, for example, feeling deserving of pain because of perceived wrongdoing or as punishment for being weak;
- a way to stop feeling numb, disconnected or dissociated;
- creating a reason to physically care for themselves;
- a ‘blackout’ – some are unaware of their actions, self-harm is an unconscious decision – a form of dissociation – when the person is only aware of the injury after their ‘blackout’;
- an expression suicidal feelings and thoughts without taking their own life.
In the video below, four people explain the reasons behind their self-harm and the different ways they have learned to cope.
Born survivors is an hour-long UK documentary which gives an insight into the phenomenon of self harming teenagers by following three young people who have resorted to it as a way of coping with what life has thrown at them. The programme may be helpful to those wishing to broaden their understanding of deliberate self-harm (DSH) and how others’ attitudes affect those who harm.
After self-harming, the patient may feel better and able to cope, however, because the original stressor is often still present, this increased mindset may not last for long.
The risk factors for self-harm are similar to those for suicide, including socio-demographic factors, significant life events, family adversity, psychiatric and psychological factors. Self-harm and suicide are behaviours, not psychiatric disorders. It is recognised that they often occur in the context of a diagnosable mental disorder, but neither is a disorder in and of itself. While there is a range of risk assessment and management tools and checklists, according to the National Institute of Healthcare and Excellence, these have poor predictive ability and should not be used in isolation to make treatment decisions. To assess whether a patient is engaging in self-harm or suicidal behaviour, a comprehensive clinical interview by a mental health professional is required. Ambulance staff and first responders need to urgently establish the likely physical risk, and the person’s emotional and mental state, in an atmosphere of respect and understanding.
According to Headspace, general principals during an assessment should include:
- Initiate a therapeutic relationship by demonstrating acceptance of the person and empathy
- Engender hope when possible
- Explore the meaning of self-harm for that person
- Clarify current difficulties
- Observe their mental state (both verbal and non-verbal features)
A psychosocial assessment should include an assessment of needs and risks. These could include questions about the person’s:
- Social and family circumstances;
- Significant relationships that might be supportive or might represent a threat;
- History of mental health difficulties;
- Current mental health difficulties;
- Use of drugs or alcohol;
- Past suicidal intent or self-harm (e.g. methods, frequency);
- Current self-harm (e.g. methods, frequency);
- Current desire to die;
- Current suicidal ideas;
- Current suicidal plans;
- Current suicidal intent;
- Access to means to end their life; and
- Coping mechanisms and strengths (e.g. things that the person has used successfully in the past to cope with other difficult situations).
Despite the widespread use of risk scales, research published in March 2017 identified that people who come to hospital after self-harm are unlikely to be helped by the use of risk scales when they see mental health staff. The study, led by Professor Nav Kapur from The University of Manchester, casts a critical light on the use of risk scales as part of assessments for people with self-injury or self-poisoning. The research identified that risk scales are no better at identifying who will go on to self-harm again than asking a clinician or patient a single question about how likely they think a repeat episode is to occur. Good quality assessment and treatment of people who present to hospital after taking an overdose or injuring themselves is a core part of clinical practice and can help reduce risk of repeat self-harm and even suicide.
The UK West London Mental Health NHS Trust produced a series of videos on mental health awareness to assist non mental-health professionals, including one on self-harm. Illustrating the pathway from home to hospital, the video is designed as an educational tool and includes discussion topics and management considerations.
It is not appropriate to dismiss self-harm as a ‘cry for attention’. To reduce the misunderstanding and stigma associated with self harm we need strategies that promote community awareness and understanding of self-harm. Strategies are also needed to respond to self-harm quickly and effectively by addressing the serious underlying issues that negatively impact on a person’s mental health and wellbeing.
Suicide and self-harm account for a considerable portion of the burden of disability and mortality among young people. As stated above, self-harm is the seventh leading contributor to the burden of disease in both males and females 10 – 24 years old (11). It is estimated that 21% of “years life lost” due to premature death among Australian youth was due to suicide and self-inflicted injury (12). In addition, non-fatal suicidal behaviour and self-harm are associated with substantial disability and loss of years of healthy life (12).
If you or someone you know needs help or support for self-harm in Australia, use the numbers below. In an emergency, call 000.
AUSTRALIAN NATIONAL CRISIS COUNSELLING AND HELPLINES
Lifeline (24 hours) 13 11 14
Kids Helpline – 24 hours, for young people aged 5 to 25 years 1800 55 1800
Reach Out – Interactive website to help young people www.reachout.com
SANE Helpline – mental illness information, support and referral 1800 18 SANE (7263)
If you are not in Australia, run an internet search for self-harm or suicide help in your locality, visit a health professional, or dial your national Emergency number if required.